American troops have departed Iraq. The drawdown has begun in Afghanistan. The Pentagon’s latest strategy document focuses on the Asia-Pacific region and the great power challenges therein. The Army and Marines prepare to grow smaller, while the Navy and Air Force increase capabilities for anti-access, area denial environments. Big war is back and counterinsurgency (COIN) is out.
Yet with almost 100 percent certainty, a time will come when the works of T.E. Lawrence and David Galula will again be dusted off along with lessons from Vietnam, Afghanistan and Iraq. A new generation of Americans will find themselves confronted by the latest strategic surprise, calling us to intervene in a foreign insurgency.
This article offers an enduring argument against involving American forces in COIN, based on a crucial factor that has hitherto received little attention: the mental health of the populations in weak and failed states. This argument suggests that successfully countering insurgencies in weak and failed states such as Afghanistan, Iraq, and a number of African nations will nearly always be doomed to failure. This position is buttressed by the high rate of pre-existing mental disorder among the populations of failed states. Said another way, the main effort of the counterinsurgency—the host nation government and security force—as well as the population, whose allegiance the counterinsurgent seeks, are both beset by mental disorder.
Central to this argument is the assertion that a nexus exists between weak and failed states, insurgencies and the prevalence of mental disorders. This paper focuses on two: Post-traumatic Stress Disorder (PTSD) and Major Depressive Disorder (depression). Furthermore, this nexus is such that, each of the three characteristics can drive changes in the others. For example, as a state becomes increasingly weak and failed, the likelihood of insurgency increases. As insurgencies and the trauma associated with them intensify, the rates of mental disorder among the population will also increase. As rates of mental disorder increase, the likelihood increases that a state will remain in its failed status. It is difficult to break free from this “sticky” situation.
This article examines the nexus between weak and failed states, insurgencies and prevalence of mental disorder; the impact of mental disorders on the individual and society; and the interaction between mental disorders and the use of military force. Finally, recommendations will be offered for senior leader consideration.
The Nexus between Weak and Failed States, Insurgencies, and Mental Disorders
The governments of weak and failed states have, by definition, become ineffective, illegitimate or both. As a result, the population’s grievances become more widespread, intense and legitimate. Weak governance is, therefore, frequently cited as a common precondition for insurgency.[1] Additionally, “when states fail, those with power employ it to extract resources from those without power. The latter flock to those who offer them security, albeit often for a price…Political predation from the top is thus accompanied by the militarization of civic society below.”[2]
Afghanistan provides an example of such a militarized civic society. Frequently, “Taliban” is incorrectly used as a catch-all to denote the various groups fighting against the Afghan government and the International Security Assistance Force. The Haqqani Network, Hizb-i-Islami, drug runners, and other criminal elements all represent examples of a militarized civic society in Afghanistan.
The study of weak and failed states began in earnest in 1994 with the advent of the Political Instability Task Force (PITF), funded by the Central Intelligence Agency and comprised of scholars from a number of leading research institutions.[3] Since that time, George Mason University (GMU), the Center for Systemic Peace and the Fund for Peace in conjunction with Foreign Policy magazine, have become the prominent organizations to study weak and failed states over time.
The Center for Systemic Peace’s State Fragility Index (hereinafter “Index”) is the most comprehensive, with a full dataset reflecting 1995 to present.[4] The Index is comprised of an array of security, political, social and economic measures of a state’s legitimacy and effectiveness utilizing data from the World Bank and United Nations, among others.
The Index suggest that once a state becomes weak and failed, it is extremely difficult to break free. In 1995, the first year for which data are available, there were 20 states listed as extremely fragile—the worst category of state fragility. As Figure 1 shows, over the 15 years of available data, only one state, Guatemala, almost made it into the top 50%, while the overwhelming majority remain in the bottom 20%. Seven of the 20 remain at war. Further, once hostilities cease, it appears 40% fall back into civil war within the first decade.[5]
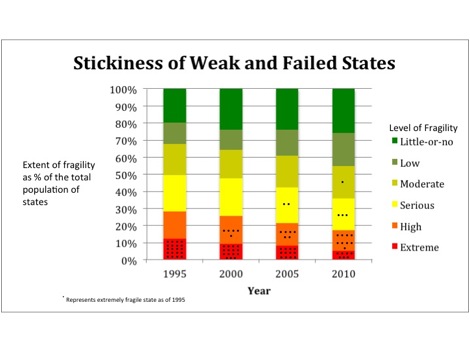
Figure 1, Tracking extremely fragile states over time[6]
The data is equally dismal in terms of the propensity for weak and failed states to be at war. Of the eight nations identified as extremely fragile in the most recent Index, seven are presently at war, compared to only one, the United States, of the 42 states assessed as having little-or-no fragility.[7],[8] As Figure 2 indicates, this relationship holds true throughout the last decade, with 64% of extremely fragile states at war during that period, compared with just 2% of little-or-no fragility states.
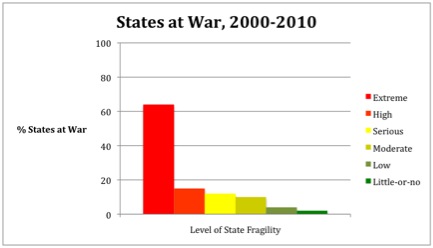
Figure 2, Average percentage of states at war each year by level of state fragility[9]
The authors of Global Report 2009 concluded that the worst category appears to be “synonymous with nearly perpetual warfare.”[10] Other researchers reached similar conclusions at the regional level. Ndulu et al found that failed states in Africa, from 1970 to 1995, were embroiled in civil wars 60% of the time. Further, of all civil wars that occurred during that time, 70% took place in failed states.[11]
The evidence is strong that the majority of insurgencies will occur in weak and failed states. Therefore, if the United States seeks to assist a foreign government in countering its insurgency, in the majority of cases it will be doing so in weak and failed states.
Perhaps not surprisingly, the populations of weak and failed states tend to reflect mental disorders, such as PTSD and depression, at significantly higher rates than those of stable states.[12] In 2009, the Journal of the American Medical Association published a meta-analysis of 181 surveys to examine the “prevalence of depression or PTSD among refugee, conflict-affected populations or both.”[13] Although the criterion for survey inclusion was not specifically weak and failed states, but rather those states subject to “armed conflict or widespread organized violence”, as noted above, there is a strong correlation between state fragility and armed conflict. Additionally, a comparison of the countries from the 181 surveys with those in the Index, revealed that weak and failed states were significantly overrepresented. For example, while extremely fragile states represent only 6% of the world’s nations, 38% of the surveys were conducted within those populations. Conversely, little-or-no fragility states typically represent 26% of the world’s nations, yet none of the surveys were done among these populations. Finally, included in the surveys were weak and failed states where American ground forces have fought, notably, Afghanistan, Iraq, and Somalia.
The meta-analysis showed substantially higher rates of PTSD and depression among refugee and/or conflict-affected populations. The 145 surveys which addressed PTSD revealed an overall weighted prevalence of 30.6%, compared with an estimated prevalence rate of 5% across the entire range of populations.[14],[15] The populations of weak and failed states, therefore, have PTSD rates approximately 500% greater than those of the average nation. The results for the presence of depression were nearly identical, with a weighted prevalence rate of 30.8% for the 117 surveys focused on depression.[16]
In terms of causation, mental disorders such as PTSD and depression are strongly correlated with traumatic events, defined in the American Psychiatric Association's (APA) Diagnostic and Statistical Manual of Mental Disorders as a situation where “the person experienced, witnessed, or was confronted with an event where there was the threat of or actual death or serious injury. The event may also have involved a threat to the person's physical well-being or the physical well-being of another person. The person responded to the event with strong feelings of fear, helplessness or horror.”[17] Examples of traumatic events include combat, forced relocation from one’s home, victimization in the form of torture and rape, and natural disasters.
Depression, aptly described as an end-product of failed adaptation to chronic emotional stress, is frequently present among those with PTSD.[18] Research indicates 30-50% of those with PTSD also display “significant depressive symptomatology.”[19] Conversely, there are those who will have depression but will not have PTSD. In the aggregate, though, a significant portion of those with either PTSD or depression will also have the other, particularly in the context of weak and failed states where exposure to trauma is recurring.
The likelihood of a person having PTSD and/or depression, as well as the intensity of that disorder, is correlated with the severity of traumatic experience, the number of traumatic experiences they were exposed to, and the time elapsed since exposure; though experts debate the contribution of each and some focus on only one or two of the variables.[20] Cumulative exposure to traumatic events has the strongest correlation for depression.[21] For PTSD, previous experiences of torture, which is defined as the “deliberate…infliction of physical or mental suffering…to force another person to yield information…or for any other reason,” has the strongest correlation.[22] For example, while the overall weighted prevalence of PTSD in conflict-torn nations is 30.6%, that number jumps to 53.5% when filtering for those with the highest exposure rates to torture.[23] Temporal proximity to the conflict, as suggested, also impacts the likelihood of PTSD and depression, with rates declining as time elapses from conflict termination. For instance, the surveys completed while a conflict was on-going or had been terminated for less than a year, yielded 39.9% rates of PTSD, while those surveys conducted two to six years after conflict termination reflected that 23% of the affected population still had PTSD.[24]
As Figure 3 indicates, PTSD rates climb dramatically in populations that are conflict-affected and/or become refugees. Additionally, these rates climb even higher when populations are confronted with high rates of terror, defined as political violence and terror so pervasive, that it affects the “majority of the population.”[25]
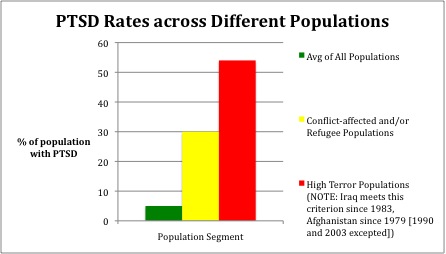
Figure 3, Prevalence of PTSD among different populations[26]
Weak and failed states provide the ideal environments—severe traumatic events, recurring and cumulative exposure, and little time since last exposure to trauma—to create dramatically high rates of PTSD and depression. And, in those weak and failed states also beset with high terror rates, PTSD levels climb to more than 50%.
Impact of Mental Disorders on the Individual and Society
Those with PTSD or depression, by the APA’s definition, have an array of cognitive and behavioral symptoms that impair their social, occupational, or other area of functioning.[27] In the case of PTSD, symptoms often include persistent re-experiencing of the traumatic event, increased anxiety, a numbing of general responsiveness, “deliberate efforts to avoid thoughts, feelings…about the traumatic event and to avoid…situations and people who arouse recollections of it,” loss of meaning, and substance abuse.[28] Symptoms for depression typically include depressed moods or lack of interest in normal activities lasting for two weeks or longer and a “diminished ability to think or concentrate;” the depressed person may also feel intensely threatened.[29] Additionally, a large body of literature indicates traumatic stress impairs learning and memory processes, which has profound implications for weak and failed states wrestling with effectiveness and legitimacy issues.[30]
Of particular concern for quelling insurgencies is learned helplessness, which is strongly correlated to both PTSD and depression.[31] Learned helplessness typically occurs after exposure to uncontrollable events and results in a person disassociating their own actions from achievement of a positive outcome.[32] They no longer perceive themselves as having control over future outcomes, so they no longer try. As a person learns that their situation is uncontrollable, cognitive, motivational and emotional deficits occur. In the cognitive domain, future learning is impaired. The person has difficulty seeing how A causes B. Motivationally, voluntary initiation of activity decreases. And, emotionally, the person’s interest levels decrease.[33]
PTSD and depression, like the statuses of weak and failed states, are persistent, even when medically treated. In the case of depression, the literature is fairly unified—remission occurs for less than half of those who receive treatment.[34] For example, a meta-analysis of 34 studies involving drug treatment indicated an overall remission rate of 38%.[35] For PTSD, the literature is more ambiguous, with remission rates recorded from less than 20% to 100%. However, a meta-analysis of 55 studies yielded a 56% remission rate for those who received treatment.[36]
In sum, mental disorders impair the individual’s functioning. Interpersonal relationships are disrupted. Cognitive deficits decrease capability. Finding and keeping a job gets more difficult.[37] And, the prognosis for recovery is quite challenging. The toll on the individual and their loved ones can be immense. When, however, the incidence rates skyrocket to 30% in the case of conflict-affected nations, or beyond 50%, as is the case in high terror states, society as a whole endures the negative effects.
Weak and failed states face additional challenges. Medical treatment is typically limited in the best of times and will be severely disrupted during conflict. Additionally, there is little hope of effective treatment if the person continues to be exposed to the same traumatic experiences that caused the mental disorder in the first place.
Military Force and Mental Disorders
In traditional war, where nation-states fight in force-on-force military operations, military force is used in concert with the other instruments of national power to defeat, destroy or seize.[38] Each of those three words from joint doctrine—defeat, destroy and seize—superbly captures the negative atmosphere of traditional war, an atmosphere so deteriorated that every instrument of power is increasingly used in a coercive manner. War is a downward slide, with the use of military force applied to accelerate the run to the bottom where, ultimately, the enemy’s fielded force has been defeated or the will of the population or decision-makers has been sufficiently shocked that they opt for surrender. In traditional war, mental disorders among the opposing population or its fielded force arguably work to our advantage. As we seek to accelerate the downward slide, increased prevalence of mental disorders further destabilizes the opposing state and its population, and destabilizing fits well with efforts to defeat, destroy and seize.
Countering insurgencies, however, is quite dissimilar. It is contained under the umbrella of irregular warfare (IW), which joint doctrine defines as a “violent struggle…for legitimacy and influence over the relevant population.”[39] Deleterious terms such as destroy, defeat and seize give way to the more constructive vocabulary of legitimacy and influence. Whereas traditional war is a downward slide accelerated by military force until the conflict is resolved, in COIN military force is used to arrest the downward slide. Accordingly, the majority of military force is dedicated to providing security for the population and increasing the capacity of host-nation security forces, while only a minority is focused on killing and capturing insurgents. According to joint doctrine, “COIN requires joint forces to both fight and build.”[40]
Joint doctrine goes on to say that what makes IW “’irregular’ is the focus of its operations – a relevant population – and its strategic purpose – to gain or maintain…the support of that relevant population…”[41] And therein lies the problem: Both the population and the government of weak and failed states suffer from such high rates of mental disorders, that accomplishing positive objectives becomes extremely difficult. Increasing government capability and legitimacy, and gaining the population’s active support are quite problematic when the government, security force and population are beset with PTSD and depression.
For the insurgents, however, the high rates of PTSD and depression provide a benefit in much the way they do in traditional war. The high rates inhibit positive growth in government legitimacy and capability, while making the population more susceptible to intimidation and the belief that they themselves are incapable of changing things for the better. While this does not endear the insurgents to the population, it does keep the environment unstable and insecure over time, which is often an insurgent goal.
If an American unit had PTSD and depression rates of 30% or higher, it would likely be declared combat ineffective. When we conduct COIN in weak and failed states, we are supporting a government and security force that is likewise combat, or perhaps more appropriately, mission-ineffective. Mentoring and training them to a sufficient level of legitimacy and effectiveness is incredibly difficult, particularly so in the timeframes likely required by domestic political considerations.
Recommendations
1. Conduct COIN only when absolutely necessary. In populations beset with mental disorders, stability and growth are strongly inhibited, while the resources required for successful COIN, in terms of time and capital, are profound. Evidence from Vietnam, Iraq and Afghanistan suggests US policy-makers severely underestimated the resources required to successfully conduct COIN in those weak and failed states.
2. Include a psychological estimate/analysis of the host nation in any COIN OPLAN and ensure sufficient mental health capability to address the mental disorders of their population. Since 2001, the military has done a significant amount of learning and adapting, including ensuring attention is paid to the host nation culture, language and history. The same cannot be said of the psychological component. Joint Publication 3-24, Counterinsurgency Operations, refers to culture and its importance nearly 100 times, while psychological considerations of the population go unmentioned.[42] Furthermore, just as we recognize the need to secure the population, we should also recognize the need to secure the psychological domain of the population. It is not compassion that drives this point, rather it is the assertion that a temporarily secured population will inevitably give way to insurgency and a continued weak and failed status if the high rates of mental disorders are not addressed.
3. Slow the speed at which sovereignty is returned to the host nation government. Joint doctrine presents a model of governance across a range of state fragility.[43] Optimally, the host nation government is in charge, and this typically corresponds with nations that are in “recovery.” When the state is “failing,” a transitional civilian government will often be in place, and when it is “failed,” a transitional military government may very well need to be in charge. While a transitional military government is described as undesirable, joint doctrine acknowledges that less desirable forms of government may be required during periods of increased fragility. As an example, Afghanistan has had an elected president since 2004, though Afghanistan was and remains stuck in the worst fragility category. Joint doctrine suggests, and Afghanistan’s current status appears to corroborate, that such weak and failed states are incapable of legitimately and effectively governing their people.
4. Only enter areas where security will be provided 24/7. While enduring security is optimal, no security or government presence appears to be preferable from the population’s perspective to only having some security and presence. Touch-and-go US or host nation presence sets up the population as targets for increased insurgent intimidation: Are you working with the government? What information did you give them? Did you ask them to come? This results in even more traumatic events. PTSD and depression rates will likely rise in response, making the situation worse than if there had been no US/host nation presence.
5. Vigorously debate the use of force in COIN. Doctrine currently recommends to “limit the use of force to the minimum necessary.”[44] This is tied to American ideals, international laws and treaties, and the belief such discretion enhances government legitimacy. In Afghanistan and Iraq, however, widespread insurgency and rampant violence occurred only after we intervened. The removal of two reprehensible regimes and the subsequent inability of the host-nations/international community to provide adequate security unwittingly ushered in the conditions necessary for the insurgencies and spiraling rates of violence. Perhaps a less limited use of force might have yielded different results.
6. Study the impact of mental disorders in COIN. Achieving America’s objectives is the focus of our military. In COIN settings, mental disorders and the broader psychological component have largely been ignored, negatively impacting our ability to achieve America’s objectives. Studies could be commissioned among the medical community, academia and think tanks; entities which have the expertise to better understand the presence and impact of mental disorders among weak and failed state populations. Such studies would better inform the planning and execution of future COIN operations.
Conclusion
This article suggests there is an enduring argument to be made against America conducting COIN. Specifically, the argument is that insurgencies often occur in weak and failed states, which are home to disproportionately high rates of mental disorders such as PTSD and depression. This results in a problematic cycle of violence and traumatic events which drive higher rates of mental disorder which, in turn, place additional pressure on a failed state to remain in that category. As a result, victory from the counterinsurgent’s perspective becomes almost impossible.
[1] Seth Jones, “The Rise of Afghanistan’s Insurgency: State Failure and Jihad,” International Security (2008), 8. See also James Fearon and David Laitin, “Ethnicity, Insurgency, and Civil War,” The American Political Science Review 97 (2003), 75.
[2] Robert Bates, “State Failure,” Annual Review of Political Science (2008), 9.
[3] Center for Global Policy, State Failure - Political Instability Task Force (19 Jan 2010), available at http://globalpolicy.gmu.edu/pitf/.
[4] By way of comparison, the Fund for Peace’s Failed State Index dataset starts in 2005. Additionally, it should be noted that early work on the State Fragility Index was done through GMU’s Center for Global Policy.
[5] Paul Collier, Anke Hoeffler, and Mans Soderbom, “Post-Conflict Risks,” Journal of Peace Research 45:4 (2008), 465.
[6] Data extracted from Marshall & Cole’s Global Report 2010 and State Fragility Index and Matrix 2010, as well as Marshall & Gurr’s Peace and Conflict 2005, Gurr et al’s Peace and Conflict 2001, and Marshall’s Major Episodes of Political Violence 1946-2011.
[7] Monty Marshall and Benjamin Cole, State Fragility Index and Matrix 2010 (2011a), available at http://www.systemicpeace.org/SFImatrix2010c.pdf, 1.
[8] Marshall and Cole (2011a), 34-35. To be at war, a state must have at least 500 "directly-related" fatalities and sustain a base rate of 100 "directly-related deaths per annum." Therefore, of all ISAF nations, only the US is at war in Afghanistan.
[9] Data compiled from Global Report 2011, 2009, 2008, 2007; Peace and Conflict Report 2005, 2003, 2001; as well as the State Fragility Index, 1995-2010.
[10] Marshall and Cole (2009), 22.
[11] Bates, 3.
[12] Zachary Steel et al, “Association of Torture and Other Potentially Traumatic Events With Mental Health Outcomes Among Populations Exposed to Mass Conflict and Displacement A Systematic Review and Meta-analysis,” Journal of the American Medical Association 302:5 (2009), 540, 543. See also Aziz Yasan et al, “Trauma Type, Gender, and Risk of PTSD in a Region Within an Area of Conflict,” Journal of Traumatic Stress 22:6 (2009) 663; and American Psychiatric Association, American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, Text Revision. (Washington, DC: American Psychiatric Association, 2000), 466.
[13] Steel et al, 538.
[14] Steel et al, 540.
[15] Yasan et al, 663; American Psychiatric Association, 466.
[16] Steel et al, 544.
[17] American Psychiatric Association, 466.
[18] Louisa Burriss et al, “Learning and Memory Impairment in PTSD: Relationship to Depression,” Depression and Anxiety 25:2 (2008), 155. See also Charles Nemeroff et al, “Posttraumatic stress disorder: A state-of-the-science review,” Journal of Psychiatric Research 40:1 (2006), 5, 8, 10; and Jon Elhai et al, “Testing whether posttraumatic stress disorder and major depressive disorder are similar or unique constructs,” Journal of Anxiety Disorders (2011), 404-5.
[19] Duncan Campbell et al, “Prevalence of Depression–PTSD Comorbidity: Implications for Clinical Practice Guidelines and Primary Care-based Interventions,” Journal of General Internal Medecine 22:6 (2007), 712.
[20] Patrick Vinck, “Exposure to War Crimes and Implications for Peace Building in Northern Uganda,” Journal of the American Medical Association 298:5 (2007), 543. See also Denise Michultka, Edward Blanchard and Tom Kalous, “Responses to Civilian War Experiences: Predictors of Psychological Functioning and Coping,” Journal of Traumatic Stress 11:3 (1998), 571, 575-6; as well as Kaz de Jong et al, “The Trauma of War in Sierra Leone,” The Lancet 355:9220 (2000), 2067; and Howard Johnson Andrew Thompson, “The development and maintenance of post-traumatic stress disorder (PTSD) in civilian adult survivors of war trauma and torture: A review,” Clinical Psychology Review 28 (2008), 40-2.
[21] Steel et al, 547.
[22] World Medical Assembly, WMA Declaration of Tokyo - Guidelines for Physicians Concerning Torture and other Cruel, Inhuman or Degrading Treatment or Punishment in Relation to Detention and Imprisonment (1975), preamble, available at http://www.wma.net/en/30publications/10policies/c18/; Steel et al, 547-8.
[23] Steel et al, 543. See also the Political Terror Scale at http://politicalterrorscale.org/ which uses US Department of State and Amnesty International data to ascribe a rating to each country based on the extent to which the government and/or its agents use political violence and terror against the population. Data is available from 1976 onwards.
[24] Steel et al, 540-1.
[25] Steel et al, 543.
[26] Data compiled from Steel et al, 540, 543; Yasan et al, 2009), 663; American Psychiatric Association, 466; and the Political Terror Scale.
[27] American Psychiatric Association, 349, 463; Nemeroff et al, 5.
[28] American Psychiatric Association, 463-4; Josh Cisler et al, “PTSD symptoms, potentially traumatic event exposure, and binge drinking: A prospective study with a national sample of adolescents,” Journal of Anxiety Disorders 25:7 (2011), 978. See also Raymond Flannery and Mary Harvey, “Psychological Trauma and Learned Helplessness: Seligman's Paradigm Reconsidered,” Psychotherapy 28:2 (1991), 374.
[29] American Psychiatric Association, 345, 356, 465.
[30] Burriss et al, 150. See also J. Douglas Bremner et al, “Functional Neuroanatomical Correlates of the Effects of Stress on Memory,” Journal of Traumatic Stress 8:4 (1995), 529; Charles Morgan III et al, “Stress-Induced Deficits in Working Memory and Visuo-Constructive Abilities in Special Operations Soldiers,” Biological Psychiatry 60:7 (2006), 726; and Slawomira Diener et al, “Learning and Consolidation of Verbal Declarative Memory in Patients with Posttraumatic Stress Disorder,” Journal of Psychology 218:2 (2010), 139.
[31] Bargai, Ben-Shakhar and Shalev, 272, 274.
[32] Neta Bargai, Gershon Ben-Shakhar and Arieh Shalev, “Posttraumatic Stress Disorder and Depression in Battered Women: The Mediating Role of Learned Helplessness,” Journal of Family Violence 22 (2007), 268. See also Steven Maier, “Exposure to the Stressor Environment Prevents the Temporal Dissipation of Behavioral Depression/Learned Helplessness,” Biological Psychiatry (2001), 763.
[33] Lyn Abramson and Martin Seligman, “Learned Helplessness in Humans: Critique and Reformulation,” Journal of Abnormal Psychology 87 (1978), 50.
[34] Diane Warden et al, “The STAR*D Project Results: A Comprehensive Review of Findings” Current Psychiatry Reports 9 (2007), 449, 451. See also Madhukar Trivedi et al, “Evaluation of Outcomes With Citalopram for Depression Using Measurement-Based Care in STAR*D: Implications for Clinical Practice,” American Journal of Psychiatry 163 (2006), 33; A. John Rush et al, “Selecting Among Second-Step Antidepressant Medication Monotherapies: Predictive Value of Clinical, Demographic, or First-Step Treatment Features,” Archives of General Psychiatry 65:8 (2008), 870; Papakostas, Maurizio Fava and Michael Thase, “Treatment of SSRI-Resistant Depression: A Meta-Analysis Comparing Within- Versus Across-Class Switches,” Biological Psychiatry 63:7 (2008), 699; and Raymond Lam, “Priorities in treating depression only,” International Journal of Psychiatry in Clinical Practice 8:suppl 1 (2004), 26.
[35] Charles Nemeroff et al, “Comprehensive analysis of remission (COMPARE) with venlafaxine versus SSRIs,” Biological Psychiatry 63:4 (2008), 426-7.
[36] William Berger et al, “Pharmacologic alternatives to antidepressants in posttraumatic stress disorder: A systematic review,” Progress in Neuro-Psychopharmacology & Biological Psychiatry 33:2 (2009), 170. See also Kathryn Ponniah and Steven Hollon, "Empirically supported psychological treatments for adult acute stress disorder and posttraumatic stress disorder: a review," Depression & Anxiety 26 (2009), 1090-1100.
[37] Jennifer Vasterling et al, "Attention, learning, and memory performances and intellectual resources in Vietnam veterans: PTSD and no disorder comparisons," Neuropsychology 16:1 (2002), 10-12. See also Karsten Paul and Klaus Moser, "Unemployment impairs mental health: Meta-analyses." Journal of Vocational Behavior 74 (2009), 278; and Arne Mastekaasa, "Unemployment and Health: Selection Effects," Journal of Community and Applied Social Psychology 6 (1996), 189, 199, 203; and Holly Prigerson, Paul Maciejewski and Robert Rosenheck, "Population attributable fractions of psychiatric disorders and behavioral outcomes associated with combat exposure among US men," American Journal of Public Health 92 (2002), 60.
[38] Joint Chiefs of Staff, Joint Publication 1: Doctrine for the Armed Forces of the United States (Washington, D.C.: Joint Chiefs of Staff, 2007/updated 2009), I-6.
[39] Joint Chiefs of Staff (2007), I-1.
[40] Joint Chiefs of Staff, Joint Publication 3-24, Counterinsurgency Operations (Washington, D.C.: Joint Chiefs of Staff, 2009), I-14.
[41] Joint Chiefs of Staff (2007), I-7.
[42] Psychological or a variant is used in JP 3-24, but the use is limited to psychological operations or isolating the insurgents from the population both physically and psychologically.
[43] Joint Chiefs of Staff (2009), I-5.
[44] Joint Chiefs of Staff (2009), III-10.
About the Author(s)
Comments
Low signature FID to address insurgencies is a way of doing business we were fairly proficient at prior to 9/11 and I think we can get back to it.
Concur on the lack of creative thinking, because the military did what it normally does, it dusted off an old manual based on an old war (Colonial rebellions) and turned it into a doctrine. What they failed to do was seek understanding of the problem/system before they came up with a solution.
Bill- I meant that I wondered why we did that more with a note of frustration as opposed to really wondering "why". I think we do it because of a lack of critical and creative thinking and we've gone lock-step into the 3-24/all things Malaya thinking (Malayan narrative according to some).
<em>"...Erik G below wonders how small scale COIN would achieve US interests in most instances."</em>
<em>"I submit that it (small scale COIN) would not. This, if US interests today are generally defined as transforming the lesser and remaining outlier states and societies as the global economy requires..."</em>
The problem with that in my opinion is that US interests are very subjective- and change with the prevailing political winds and fickleness of the nation. Sometimes what would seem to be in our interests today were definitely not something that we thought were in our interests in the past and vice versa.
So- I would submit that depending on the context- including the current political masters' take on things- doing small signature COIN- COIN defined as us assisting another with their COIN which is different than the overarching concept of FID- <em>would</em> be in our interests- and much more so than doing nothing or attempting nation-building.
If you follow the line of reasoning that in the long run what is more resilient for a country are those things that they come up with themselves and that it is very difficult in many instances to figure out what IS in our nations' interests during internal conflicts- then low-signature COIN should be very appealing- even if the vision is one of a world of free market and democratic states all sharing in the global economy.
G. Martin below says he does not understand why we couple COIN with nation building or even stability operations.
I suggest that the reason we do this (couple COIN with nation building and/or stability operation) is so that we might use the opportunity presented by the insurgency -- and/or other forms of instability -- to transform lesser and remaining outlier states and societies as the global economy requires (to wit: along modern western lines).
Erik G below wonders how small scale COIN would achieve US interests in most instances.
I submit that it (small scale COIN) would not. This, if US interests today are generally defined as transforming the lesser and remaining outlier states and societies as the global economy requires.
Today, the primary obstacle to world peace and prosperity is no longer believed to be of the great power variety. These folks are all pretty much on the same sheet of music that we are (to wit: all are significantly market-focused, market-oriented and market-dependent).
The primary obstacle to world peace and prosperity today is believed to be those lesser and remaining states and societies who have other priorities -- and/or other interests -- and who, as such, have yet to become sufficiently organized, oriented, ordered and configured as the global economy requires.
In the old days, it was the contrary non-market/non-western orientation of certain of the big guys (certain of the great powers) that gummed up the works.
Today, it is the different focus and orientation of certain of the little guys that make things more difficult than they otherwise need to be.
Thus, (returning to G. Martin's thought above) nation building gets connected to COIN to try to overcome this problem of lesser and remaining states and societies not be organized, oriented, ordered and configured as the global economy requires.
And (returning to Erik G's concern above) small scale COIN is understood to be insufficient to getting this (fundamental and complete state and societal transformation) job done.
(The financial crisis, however, putting all of this on hold for the time being.)
Bill -
Ref. your comments:
- "It is the host nation's fight (political and military) to win or lose, if they fail to take the needed actions, or lack the political legitimacy to do so, then they can't win." Amen.
- "When they can't win is when we tend to make what in hindsight appear to be very dumb decisions about surging our forces and in fact taking the lead, that is when we own the problem and it is our fight to win or lose. That in itself seems to be form of mental illness, we realize the HN can't win for a variety of reasons, so we decide to prompt them up with our military forces and then wonder why the people we think we're trying to help are turning against us." I almost busted a gut. Well said! To share a quick example, it took me a fair amount of time before I realized the key Afghan government official I was partnered with viewed any other GIRoA official's success as a threat to him. Everything was zero sum. Before I understood that, I would praise the efforts of various officials during our meetings, thinking he'd be proud of his subordinates doing so well. Instead, it only ensured he targeted them for moves or otherwise sought to slow them down. Once I figured it out, I never praised another official except for the one guy we were desperately trying to get fired.
Erik, Grant may disagree, but I think he is describing what we do as FID, and what the host nation is doing as COIN. We had many successes with FID with relatively small forces from Greece to El Salvador and even Ed Lansdale's assistance to Magsaysay in the Philippines. I think the correct way to frame it in these situations is "we" don't change the situation/problem, we provide minimal assistance to the host nation so they can change the situation/problem. This assistance can and has included U.S. combat operations ranging from raids to now UAV strikes, but we are not the decisive force and we don't take ownership of the problem if it is true FID. It is the host nation's fight (political and military) to win or lose, if they fail to take the needed actions, or lack the political legitimacy to do so, then they can't win. When they can't win is when we tend to make what in hindsight appear to be very dumb decisions about surging our forces and in fact taking the lead, that is when we own the problem and it is our fight to win or lose. That in itself seems to be form of mental illness, we realize the HN can't win for a variety of reasons, so we decide to prompt them up with our military forces and then wonder why the people we think we're trying to help are turning against us.
The majority of future fights will unlikely look like Iraq and Afghanistan, they'll be smaller scale operations dispersed over many different countries where we'll conduct limited combat operations and persistent advisory efforts to address "common" threats. The challenge will be when it is in our security interest to eliminate a specific threat and the host nation government is simply making the problem worse with an inept approach (not that we don't apply our own inept approachs on occassions). I think it is time we move the conversation beyond the COIN doctrine and discuss other approaches to irregular threats.
One of my many unpopular views is that the Army and Marines to some extent are trying to describe these challenges around the globe in a way that requires large conventional forces to counter in order to justify current force structure. This doesn't seem to be based on honest analysis. We need a credible Army and Marine force structure to fight battles, it is questionable if we need a large GPF force structure to address Al Qaeda in Africa for example.
Bill M.
Your second sentence, second paragraph:
"First off we're pushing a system, not imposing it."
If we have invaded a country, defeated this country's military, overthrown this country's government and installed our preferred governor(s) and our preferred form of government in its place. And if we have instituted a very heavy-handed, extensive and expensive approach called "Whole of Government" to fundamentally and completely transform the subject state and society as we might desire,
Then can such an approach to state and society transformation best be described as "pushing" or would "imposing" (of one's way of life and way of governance) upon others be a more accurate way to characterize and describe what is being attempted?
(Counterinsurgency, in this context, to best be understood as a continuation of this "imposition" process. This being the phase in which the foreign entity -- and its now well-paid local partners -- attempt to overcome the resistance of the population generally to this transformation of their state, society and way of life. This phase of the operation being understood, thus and appropriately, as "war amongst the people.")
So: Can a foreign entity with a relatively small and short-term commitment (less than occupation for 50 to 100 years) -- and/or a local government with only the assistance of a "minor outside force" -- reasonably expect to be able to impose a new way of life and new way of governance on a resistant population? Maybe only, as you have said, in the foreign entity's (ethnocentric?) dreams.
Bill C.
I guess a case can be made that AQ and like minded groups are pursuing a change in political, economic and social systems in the countries they're operating in. It also not unlike what the communists did at even a deeper level, and the Conquistadors among many others. Their methods have greater efficacy at least for the short-term. These methods include: mass re-education camps, killing off those who don't reform (Mao's purge), imposing systems that direct the people what God will be worshiped (or that there is no God), and they impose the law the land upon the people.
We on the other hand are pushing a very different system and in a very different way. First off we're pushing a system, not imposing it. That is admirable, but it is also messy. Second, we're pushing self-determination (as long as you're not an Islamists, a commi, or Conquistador), so imposing a set of laws, forcing people into re-education camps, and killing off those who non-violently oppose this idea are not, nor should not be options. That brings us to your question, is COIN the right venue to achieve our vision? If our policy is based upon a fairy tale view of the world instead of reality it is doomed to fail. That policy seems to be if by using a strategy informed by our current COIN doctrine that if we create enough political and social space that all peoples will naturally drift towards our vision of an ideal society. Again, if that premise is wrong, then our strategy is doomed to fail.
Thus, in the scenerio I have offered above, what we would appear to be doing could not be called counter-insurgency -- any more than it could be called counter-terrorism, counter-humanitarian crisis, counter-genocide, counter-poor response to natural disaster and/or counter-killing of one's own people. That would not seem to be what we are doing.
Rather what we would appear to be doing is significant and fundamental state and societal change; this, so as to address the perceived central condition that is believed to give rise to all these such problems, to wit: the lack of the state and society being ordered, organized, oriented and configured along modern western lines.
Herein, should we say that is unlikely that this job/mission (the significant and fundamental change of a state and societies political, economic and social systems and, thereby, the population's way of life) can be achieved via such concepts as COIN and/or FID?
"If it is true that the majority of insurgencies occur in weak and failed states ..."
What is believed, I think, is that the majority of insurgencies -- and the majority of instances of terrorism, humanitarian crisis, genocide, poor response to humanitarian crisis and "killing of one's own people" -- this all is believed to occur in states and societies that are not adequately ordered, organized, oriented and configured along modern western lines.
Thus, the question in the minds of individuals who believe this to be true is:
a. Not "how could a minor outside force be sufficiently helpful to change the problem set of weak and failed states?" But, more specifically:
b. How could a minor outside force be sufficiently helpful to change the problem of a state and society not being sufficiently ordered, organized, oriented and configured along modern western lines?
If it's true that the majority of insurgencies occur in weak and failed states, how will a few guys on the ground be a sufficient assist to foreign troops? To become a weak and failed state, the government typically has either lost its monopoly on the use of force within its borders or it has become so illegitimate that the people rise up against it. How could a minor outside force be sufficiently helpful to change that problem set?
I'm not arguing for large COIN, but wondering how small COIN would achieve US interests in most instances.
I have to echo COL Maxwell's points. I don't understand why we couple COIN with nation-building- or even stability ops. I agree- full-blown COIN, "industrial" COIN, or nation-building- whatever you want to call it- should be debated vigorously and executed rarely- but COIN in general really assumes that a semi-viable nation state is capable of conducting COIN and we are simply assisting them due to some related national interest.
When we think of COIN- I submit- it shouldn't be something we normally associate with full-scale efforts- that, in my mind, is "COIN+": COIN + nation-building, which is an endeavor best left alone in my opinion- as it is costly, long-term, and difficult to associate with clear national interests. Simple COIN can be done with as little as one person- and him not even being in country- but could also be accomplished very much "on the cheap", the costs and efforts balanced with the clearly defined national interests at stake.
When I think of COIN- the picture in my mind is a few guys on the ground assisting foreign troops with their counterinsurgency efforts- maybe one assisting with operational level planning and the rest with some tactical tasks. Outside of that- the strategy is one developed by the host nation, we constantly monitor whether the policy that influences that strategy is in line with our nations' interests and whether the means the host nation uses is tolerable to our politicians.
I'd even go so far as to say a punitive expedition- COIN "lite" maybe- in the case of Afghanistan may today have resulted in a much more stable entity than the one we've been assisting with. I suspect that bottom-up emergent efforts- especially in the case of institution building and nation building- are much stronger than systems forced down from the top (and from external parties).
First, COL G- Hi. I think we were at Atterbury together. Aug-Oct 2010. I was in Khost PRT.
Next, although I have only just skimmed this article, it got my attention. As we speak I'm working on our reading list here (Navy-MCAST) and here are a couple books that support your thesis:
Edgerton, R. Sick Societies. The Free Press, 1992
Strange, S. The Retreat of the State Cambridge University Press, 2008
-----------------------
V/R,
tom
Erik,
I am not a supporter of COIN. And our doctrine currently makes assumptions on how the population of any given area is going to respond to our side, the host nation and the enemy. Where it fails in my opinion is that it assumes that the people see our way as being better... There is really about five ways the population can go.
1. Think our way is best
2. Think the enemies way is best
3. Think neither is worthwhile and take a third route
4. Continue to sit on the fence and watch trying to figure out who the winner is going to be so they don't support the wrong side and pay when we leave.
5. Want to be left alone, by all sides
As for limiting force being an american ideal... That is recent development... And since we have adopted this utterly stupid idea, we have not decisively won a conflict of any real size. I would compare the limiting of force during war as, as foolhardy an idea as limiting the amount of water used to put out your house if it is on fire... No I am not saying nuke em, til they glow, but limiting force etc has never worked. It created safehavens for the enemy in Vietnam and the same has thing has happen in Pakaistan, leaving us in an MMA bout while only being allowed to punch with one hand.
Besides we are not talking about a 10 million or even a million. In Afghanistan I will bet the enemy is a few thousand and no more... We should be able to take that amount out without worry.
Towards the end of the article, I included a recommendation to "vigorously debate the use of force in COIN. Doctrine currently recommends to “limit the use of force to the minimum necessary.” This is tied to American ideals, international laws and treaties, and the belief such discretion enhances government legitimacy. In Afghanistan and Iraq, however, widespread insurgency and rampant violence occurred only after we intervened. The removal of two reprehensible regimes and the subsequent inability of the host-nations/international community to provide adequate security unwittingly ushered in the conditions necessary for the insurgencies and spiraling rates of violence. Perhaps a less limited use of force might have yielded different results."
It's a tough nut to crack. As you discuss above, the amount of force used is an important consideration. If social norms, group interests, etc are too different between us and the population than a gap certainly seems to exist in terms of how you accomplish your objectives. The use of force is one way to try and close the gap.
Sir, "I am talking about places like slums etc. Where survival (maybe not to the level of needing to make fire) has become a fact of life," resonate for me. Those areas of our country that you reference appear to persist, generation after generation, despite the efforts expended to help and improve."
I am no pro in this area, but you are correct, these areas seem to continually exist, dispite whatever we have done to attempt the fix. I would put this idea forword. Habitat, combined with economic, educational opportunities, family situations etc seem, at least at a glance to be factors. And I think anwer to a good portion of what we see in those areas.
However I would also say those areas are havens for social norms, that have gone out of favor with the mainstream. (Feel free to correct me at any point) but street gangs are most often found in these areas. And while narcotics sales are often what they do among other things for a living, at least on the lower end, you see a tribal mentalty. A mindset much more often seen in other parts of the world. They have special language, symbols etc. that to the lay person mean nothing, but to someone else with a similer mindset they are as obvious as billboards. Much like a dog peeing on a fire hydrant, most people would and will never know what they mean, but another dog will.
My argument is this. What do these tribes respect? What keeps them in line? The reason I bring it up is, that we (the US) much like the police are not going to be able to stay out of these areas (or countries), though it might be in our own personal best interest to do so.
About the only thing that I have seen that works in a tribal, Dog Pack mentality is a Bigger, Stronger, better armed and not afraid to use it tribe or a bigger more bad ass dog. Fear is what keeps them in line, I think this is why like it or not dictators (no I am not pro dictator) have the best chances of keeping peace in these countries. I am not saying they are good for the people, economy etc. But they do have the ability to cut down lawlessness etc in those areas. How? They are the big "tribe" with the guns, who make the rules or break them as needed.
Once again and I have said this before, if we are to be sucessful in these areas, we are going to have to strike total fear into the hearts of them. After that has been done, we may be able to get them to do some reasoning. But that lasts only as long as they fear us.
Your comments, "I think if you look at "failed areas" in our own country, you see these elevated levels as well. I am taking about place like slums etc. Where survival (maybe not to the level of needing to make fire) has become a fact of life," resonate for me. Those areas of our country that you reference appear to persist, generation after generation, despite the efforts expended to help and improve. The elevated MD levels seem tied to the persistent failure, creating a problem set that is incredibly challenging and requires so much time and resources.
Sir, thanks for the response. As I said I was not trying to be flip. And I have not the background that you do in this area. But I do take the time to look around. Similar to what I said in my first comment, I think if you look at "failed areas" in our own country, you see these elevated levels as well. I am taking about place like slums etc. Where survival (maybe not to the level of needing to make fire) has become a fact of life. What do we see in these areas? We see behaviors that would be considered not the norm. But is this due to it not being normal or is this due to us, having put protective mechanisms in place that insulate us from such behaviors? What if we remove those, what would happen? I think that we are going to have to except that we got it pretty good and that most of the rest of the world does not. Therefore we are going to have to train ourselves to deal with that. In this country death used to be a family matter, you might have even built the coffin, prepared the body for burial, etc. Now a lot of parents don't take the kids to the funeral. And mental health profesionals to large extent have supported this. So what do you end up with? Well you end up with 17 thru 26 year olds who have never seen a dead body before. Combine this with the stress of combat and the first time they see on being under the worst conditions possible and you have nothing but a reciepe for PTSD, in my opinion.
Hammer999,
Interesting analogy. In terms of the mental health picture for much of the world, the MH experts suggest the "normal" rate for PTSD is about 5% (can't remember, but think depression was similar), and that increases to the rates are linked to the level and intensity of the trauma (whether in their family, town, country, etc). As trauma rates increase, the mental disorder rates appear to as well, so they find higher rates in countries that we would label as weak and failed. Those rates increase even more when the weak and failed state is also home to high levels of terror among the population.
I enjoyed your comments on being reduced to certain levels of behavior as a means of coping with their environment to survive. I think that is an area our country should closely examine before committing troops to future engagements. When we provide periodic or temporary security in an area, I'd argue we're actually increasing the trauma for the population since they're still exposed to the insurgents and, you could argue, the insurgents apply even more pressure after we've departed.
Most of the Afghans I spoke with seemed happy with the Taliban at first because finally someone provided security--there were no more shakedowns on the road, marauders at night, etc. But when they saw the Taliban excesses, they began to hate them. Even so, they tended to continue passively support them because they knew the Taliban would harm them while they knew we wouldn't. That's how many seemed to cope--do not partner with the government or ISAF because you'll become a marked man, partner with the insurgents to the least extent possible but enough not to get yourself or your family harmed.
Best wishes,
Erik
It is not my intent to sound flip here. But I would argue that the level of mental heath you describe is normal in much of the world. And was even in the US until a hundred years ago. Would that not make it the normal human condition? And if so then we are lucky to be living on cloud 9...
I am no expert in this area. However I am forced to think of this as one might a wild animal. Wild animals are the norm and we humans have domesticated animals from the wild. Being that domesticated animals lack many of the stressors of wild animals, they grow bigger, have better personalities etc, than there wild counterparts. However, if you throw the domesticated animal out of the barn and into the wild and it makes it thru the intial shock and isn't eaten by wild animals, it won't be long before it is unrecogizable as a once domesticated animal. It grows into or is reduced to this level as a means of coping with it enviroment and survivial. If the majority of the population of the world is mental, then that is the normal condition.
Sir:
The perceived problem, I believe, with the idea of
a. "... conducting a punitive expedition, taking a conventional surrender from the remnants of whatever was left, pledging our support to their new nation, and then letting them get on with rebuilding their own nation however they see fit -- with the caveat that if they allow what previously happened to occur again we will take decisive action again," and
b. The concept of sovereignty and self-determination generally,
is that these may do nothing for -- but rather tend to stand in the way of -- the transformation of various states and societies as the global economy requires.
Herein, the rise of the most powerful non-state actor -- to wit: the global market -- (1) driving this train and (2) being considered, by some, as the primary reason for the demise of the nation-state.
This helping to answer your stream of consciousness thought issues/questions as to:
a. Why someone might wish to take away sovereignty (neither present regime nor self-determination provides for the state and societal changes that the global economy requires)? And
b. What comes after the nation-state system? Answer: A system based on market-states (Philip Bobbitt - Shield of Achilles)?
What these folks are forgetting -- and/or are underplaying, I believe -- is that there are other, very powerful forces still "in play," and that these forces are likely to work, individually and/or collectively, to keep, or to put, the market back in its place.
Another contribution to the debate that will likely go on for years to come. However, I would like to take exception to one recommendation and provide some quick stream of consciousness thoughts:
QUOTE 3. Slow the speed at which sovereignty is returned to the host nation government. Joint doctrine presents a model of governance across a range of state fragility.[43] Optimally, the host nation government is in charge, and this typically corresponds with nations that are in “recovery.” When the state is “failing,” a transitional civilian government will often be in place, and when it is “failed,” a transitional military government may very well need to be in charge. While a transitional military government is described as undesirable, joint doctrine acknowledges that less desirable forms of government may be required during periods of increased fragility. As an example, Afghanistan has had an elected president since 2004, though Afghanistan was and remains stuck in the worst fragility category. Joint doctrine suggests, and Afghanistan’s current status appears to corroborate, that such weak and failed states are incapable of legitimately and effectively governing their people. END QUOTE
I think we should first not try to ever take away sovereignty so that we do not have to worry about "returning it." I say this because when we "take" a nation's sovereignty we tend to default to trying to re-create that nation at least somewhat in our image. With all due respect to GEN (RET) Powell, I think the "you break it you buy it" mentality has got us into quite a bit of trouble.
We could have conducted a punitive expedition into Afghanistan and even Iraq and instead of trying to occupy and re-build it in (at least partially) our image we could have tried to take a conventional surrender from the remnants of whatever was left, pledged our support to their new nation, and then let them get on with rebuilding their own nation however they see fit with the only caveat that if they allow what previously happened to occur again we will take decisive action again. The problem with "returning the sovereignty" to a nation is we become the judge of when they are supposedly ready and of course when we are trying to re-create their nation (again at least partially) in our image we tend to be very critical judges and like the recommendation above think that their sovereignty should be returned more slowly. And our arrogance shows through when we think we can judge what is best for another country vice letting them getting on with governing themselves. The question concerning Afghanistan is did we make it a failing state by our actions and would Afghanistan have been better off if we had allowed for the reestablishment of Afghan sovereignty immediately and allowed the Afghans to determine their own way ahead? Of course that question can only be rhetorical and is unanswerable. But it is one I think we should consider if we are ever again to undertake the adventures of large scale expeditionary interventions (and perhaps such considerations might make us think more than twice on whether to embark on such adventures).
I think sovereignty is one of the most important aspects of the international system and of course with the rise of powerful non-state actors it has come under attack and many posit the end of the Westphalian system and the declining importance of the nation-state. To which I ask – what comes next? What comes after the nation-state system? If we cannot foresee that or if what we foresee is not so good, then perhaps we should be working to strengthen and make work the nation-state system.
Although I would argue against projecting values I think there are two concepts we should consider providing US support to: one is the protection of sovereignty and two is the protection of the right to self-determination. And of course in times like the Arab Spring those two concepts might be incompatible though I think the second should take precedence internally to a nation and the first should take precedence externally.
Just to add some fuel to the fire.
